 In case your patient only reports buttock pain, there can be a huge variety of underlying pathologies making a diagnosis very challenging. Of course, we have an extensive list of provocation tests for piriformis syndrome on our channel as well. Check out our playlist with videos that can help you with that by a click on the info button in the top right corner.Īfter ruling out radicular syndrome, we would continue with provocation tests that stretch or contract the deep gluteal muscles in an attempt to elicit sciatic nerve pain. If this is the case, you first need to rule out lumbosacral radicular syndrome. So how can we perform a structured diagnosis for piriformis syndrome?įirst, make sure that your patient also suffers from symptoms of nerve root compression, so he or she describes pins & needles, burning, possible loss of feeling and strength, or shooting pain in the distribution of the sciatic nerve which runs all the way down the backside of the leg into the foot. In patients that do undergo medical imaging or surgery, most cases turn out to be caused by nerve root compression. The diagnosis makes sense from an anatomical point of view, but both are a diagnosis of exclusion and are highly debated by experts in the field. In many regards, the diagnosis of piriformis syndrome in the lower limb is comparable to thoracic outlet syndrome in the upper limb. 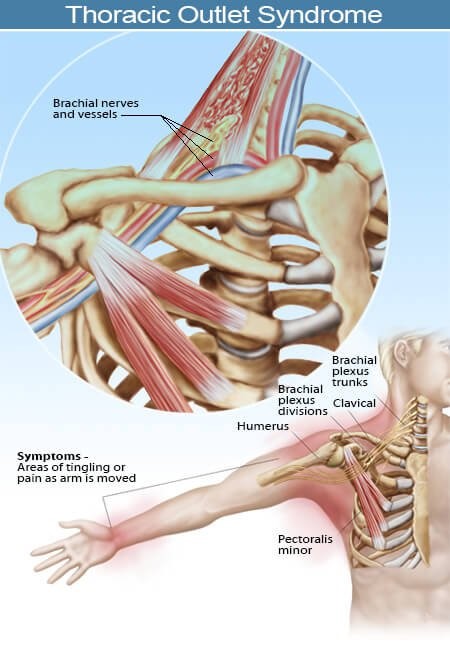
This means that in the vast majority of cases, there will be different underlying reasons for sciatica, mainly nerve root compression due to lumbar disk herniations or foraminal stenosis. So if the pain stays in the buttock area and has a quality different from nerve pain, how can the sciatic nerve be affected?ģ. In patients that do actually suffer from real sciatica, only 6-8% are thought to have piriformis syndrome. Nerve pain usually has a burning, electric, or shooting quality – most people that we see in practice only have deep, aching buttock pain and no symptoms distal to the buttock and referred pain to the posterior thigh at most. When a nerve gets compressed and irritated, patients report symptoms like pins & needles or a loss of feeling and strength in the distribution of that nerve. Piriformis syndrome by definition is the compression of the sciatic nerve by the piriformis muscle. They found no relationship between sciatic nerve variants and piriformis syndrome.Ģ. (2018) examined 1039 adult hips on MRI of which around 20% had sciatic nerve variants that might make the sciatic nerve more susceptible to compression by the piriformis muscle. Independent of how we want to call it, why do we say that it’s not piriformis syndrome then? Here are 3 strong arguments:ġ. 
For this reason, experts now prefer the term “deep gluteal syndrome”. However, there are more anatomic structures that could potentially compress the sciatic nerve like the Gemelli-obturator internus complex, the hamstring muscles, fibrous bands containing blood vessels, vascular abnormalities, and space-occupying lesions. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
